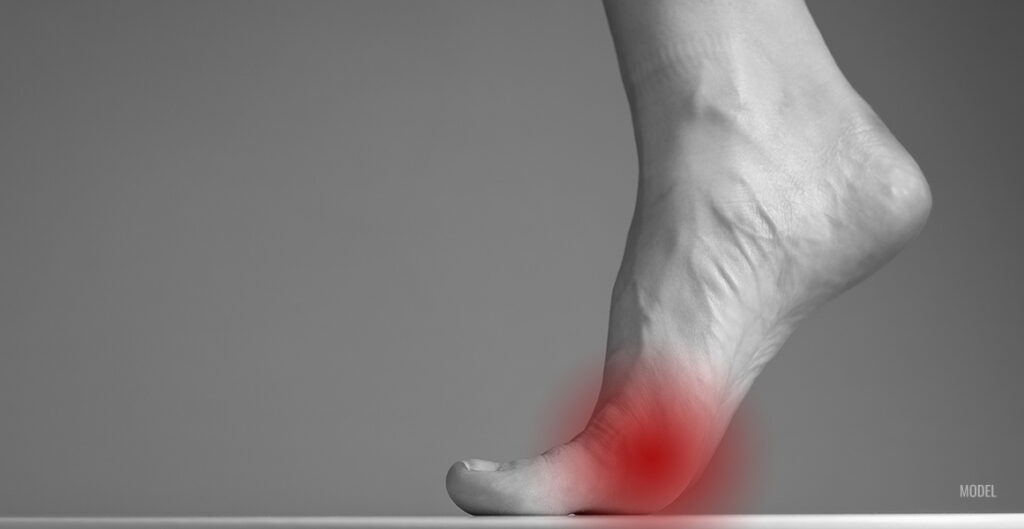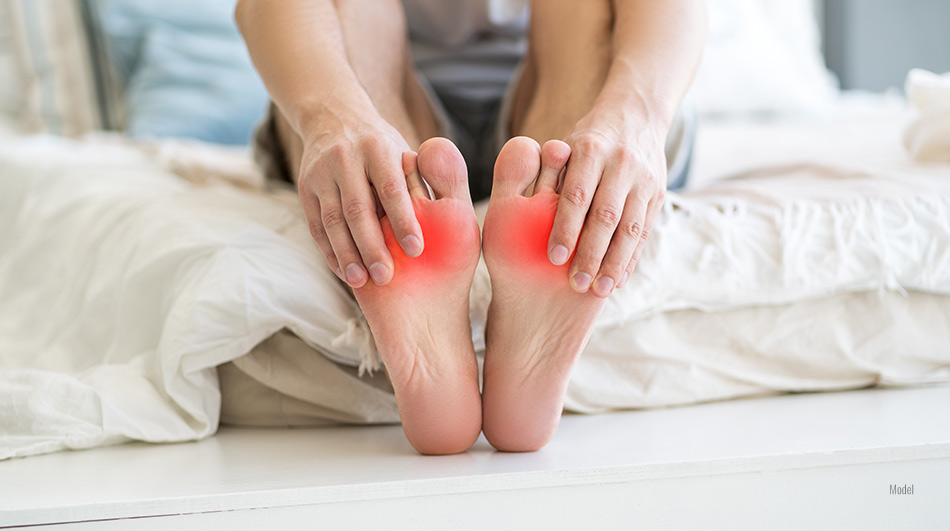
What Does Bunion Pain Feel Like?
Posted April 18, 2024 in Bunion Pain
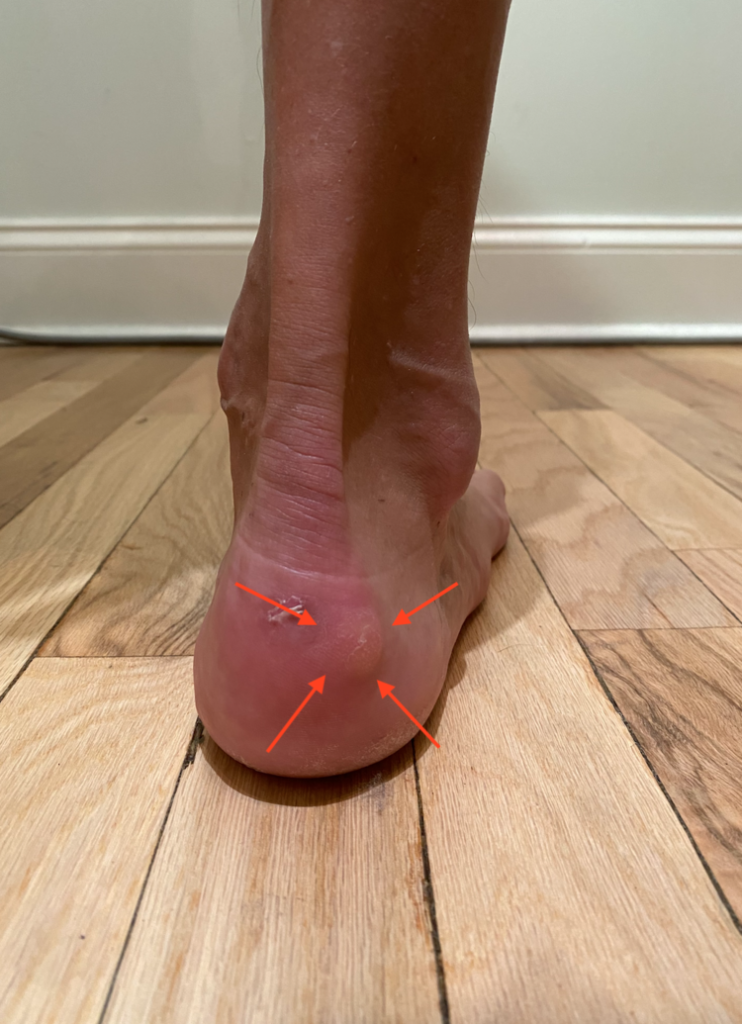
This blog discusses the basics of bunions: what they are, how they’re formed, and how to tell if foot pain is from bunions. 3 Min Read: How to Tell If You Have a Bunion People take walking around comfortably for granted until it’s gone. If you walk a lot, as many New Yorkers do, you’re […]
Read More